This page is currently being fundamentally revised. You will soon be able to find comprehensive information about your situation here and actively contribute to optimizing your healing time. We apologize for the current restrictions.
Avoid mistakes: The wound will not heal without perfect surgery
Optimal wound healing starts with choosing the right surgical method and an experienced surgeon . The more that is removed during the operation, the greater the challenge for your body to heal - a process that should not be underestimated.
Many patients initially try surgery at their nearest hospital, thinking they will only go to a specialist if they have a problem. This approach can lead to an unexpectedly long recovery time and time off school, work and sport. Our advanced therapies are designed to avoid such problems. Find out about other patients' experiences and reviews before making your decision. A long journey to a specialized facility usually pays off.
Already had surgery? Your checklist for follow-up treatment
Have you had an operation on Pilonidal Sinus and are unsure how to deal with the wound properly? It is understandable that you are confused by the numerous opinions from doctors, friends and on the internet. Our wound healing checklist summarizes what is really important. The success or failure of an operation at Pilonidal Sinus is decided in the first 4 - 6 weeks after the procedure.
Stocktaking: Was the operation performed suitable to heal the fistula?
Was your treatment aimed at removing an Pilonidal Sinus or was an abscess simply split? Even if you feel symptom-free at the moment, a second procedure is usually necessary. Without this procedure, the risk of abscess recurrence remains high.
This was only the first of two steps: Examples of abscess drainage

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
This is not how it should look: Examples of incomplete fistula removal
Have you had a complete removal of the Pilonidal Sinus performed? It is important to carefully inspect the entire gluteal fold to ensure that no noticeable openings have been left behind. The presence of such openings can be a clear sign of impending recurrence. If you suspect this, take the initiative immediately and consult a doctor who specializes in this matter.
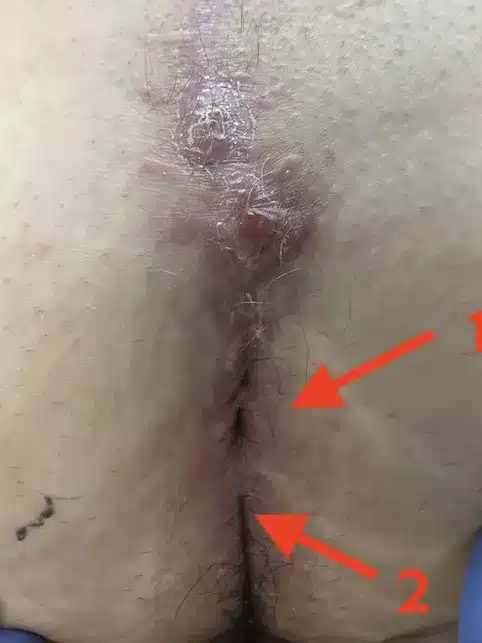
Unfortunately, this is not uncommon: despite repeated operations under anesthesia, the origin of the fistula remains unnoticed. This means that it cannot heal.

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
Basics of wound healing
After an Pilonidal Sinus operation, different priorities need to be set for follow-up treatment depending on the procedure. It is helpful to know what physiological processes take place in the body when a wound heals.
Primary wound healing with closed procedures (midline suture, Karydakis surgery)
In primary wound healing after surgical procedures with wound closure, the wound is sutured, stapled or glued. Healing then goes through four phases:
- Coagulation phase (day 1): This is when blood platelets and coagulation factors stick the wound together. The resulting fibrin is the body's own superglue. Antibodies and white blood cells are active in the defense against infection. Cohesion is primarily ensured by the skin sutures, which is why strain should be avoided.
- Inflammation phase (day 1 - 4): Messenger substances are released that cause vasodilation, increased blood flow, new blood vessel formation and the attraction of connective tissue cells (fibroblasts). These fibroblasts are true masters in the production of stabilizing fibres. The increased blood circulation can be recognized by the reddish or purple color of the scar. The mechanical stability is still low.
- Proliferation phase (day 5-14): The fibroblasts multiply and form procollagen. This protein transforms into tropocollagen and contains larger amounts of the amino acids lysine, glycine and proline. The collagen fibrils formed by cross-linking these proteins give the scar mechanical strength.
- Contraction phase (day 15 -): During this phase, the formation and breakdown of collagen fibrils are in balance and the fibers rearrange themselves. The mechanical strength of the scar continues to increase, while the color gradually returns to the normal skin tone. The scar contracts and takes on a more compact structure. The scar is now fully resilient again.
Secondary wound healing in open procedures ("Metzger" method, pit picking, sinusectomy)
Open wound treatment with secondary wound healing is usually chosen for an Pilonidal Sinus operation. Here too, the healing process goes through the stages mentioned. Between phases 2 and 3, the wound must first fill up before it can consolidate in phases 3 and 4. This takes place in the granulation phase (proliferative phase): New blood vessels (angiogenesis) form to supply the tissue with nutrients and oxygen. Fibroblasts migrate into the wound and produce collagen, which serves as a scaffold for the new tissue. Granulation tissue is formed, which consists of newly formed blood vessels, collagen and other connective tissue components. The wound fills with this tissue from the bottom up. Mechanical resilience is ensured at all times.
Follow-up treatment in detail
Effective aftercare and wound care
- Remove the hair around the wound in an approximately 2 cm wide seam by shaving, depilatory cream, waxing or plucking. Particularly important is the area 3 cm below the deepest wound point, an area that you can see by pulling the buttocks slightly apart.
- In addition, showering once or twice a day is essential to remove wound secretions and minimize the bacterial load. A clean skin surface harbors 10,000 times less bacteria and promotes faster and safer healing. Focus all your attention on these two points to optimally support the healing process!
- Wound irrigation with sterile solutions (physiological NaCL solution, antiseptics) corresponds to the official recommendation of the RKI, but in our view is not absolutely necessary. The sinusectomy procedure does not leave a poorly drained abscess cavity, but a largely "clean" wound cavity due to careful removal of the fistula capsule.
- Instructions for proper wound cleansing and care
- Use of special wound dressings and bandages
- Tips for avoiding infections
- Hair Removal
When the hair is removed, the fistula will heal.
1965 Peter H. Lord and Douglas M. Millar, pit picking inventors
Diet and lifestyle
- Nutrition tips to support wound healing (e.g. high-protein diet, vitamins)
- Importance of sufficient fluid intake
- Smoking cessation and its influence on healing
Pain control
- Pain management and suitable painkillers
- Alternative methods of pain relief (e.g. cooling, relaxation techniques)
Activity adjustments
- Recommendations for physical rest and movement restrictions
- Tips for returning to everyday life and sporting activities
Hygiene and clothing
- Suitable clothing and underwear to minimize friction and pressure
- Hygiene measures in everyday life to keep the wound clean
Warning signs and complications
- Recognizing signs of wound infection or other complications
- When to see a doctor
Scar care and cosmetic aspects
- Methods for reducing scarring
- Use of scar ointments and creams
Psychological support
- Dealing with emotional and psychological stress after surgery
- Support through self-help groups or psychological counseling
Long-term prognosis and relapse prevention
- Long-term prognosis and options for preventing recurrence
- Tips for preventing recurrence of fistulas (e.g. hair removal in the affected region)
Testimonials and patient forums
- Exchange experiences and tips with other affected people
- Access to online forums and self-help groups
You can safely omit these measures
- Antibiotics can be helpful in the short term, especially after complete closure of the wound. The first dose is typically administered during induction of anesthesia, either as an infusion or as a tablet on the morning of the operation. However, the continuation of this treatment over a longer period of time is controversial among experts. Preventive antibiotic administration to avoid wound infections should generally not last longer than three days.
- Tamponades often prove to be painful and ineffective. After removal of a fistula, the wound is usually relatively clean and should not be kept open artificially. This differs from the treatment of an abscess, where it may be necessary to ensure the drainage of pus for a few days.
- The removal of hypergranulations, also known as "wild flesh", with cauterization (silver nitrate) or mechanically is counterproductive. These growths are an indication of obstacles to healing caused by ingrown or loose hairs and are therefore a side effect and not the cause of the problem.
The wound is not healing or has reopened?
Don't leave your wound healing to chance - act now!
Plan B for stagnant wound healing: Despite inconspicuous ultrasound findings and optimal care, it can happen that a wound does not heal. If no healing progress is visible over a period of one to two months, you have to face reality: Further surgery may be necessary. Consideration may be given to re-cleaning the wound or performing a Karydakis plasty.
Do not delay the decision to undergo plastic reconstructive surgery unnecessarily. Delays only lead to loss of time and disappointed hopes. You should also not be overly afraid of the procedure. If it is performed by an experienced surgeon, it can be an effective and permanent solution to your wound healing problem.
Sport after coccygeal fistula surgery
Sport is a real health booster - even for patients after an operation! The fast-track concept of surgical rehabilitation builds on precisely this.
We have learned that bed rest, plaster casts and food restriction are not beneficial, but can actually be detrimental (keyword: inactive atrophy and catabolic metabolic states).

Open wound treatment: sport allowed without restrictions Closed wound treatment: Sport after 2 weeks
Which sports are problematic? Which are recommended?
Literature: Coccygeal fistula and sports
DR. BERNHARD HOFER & FLORIAN LIEBL
Specialists in Visceral Surgery and Proctology - PartG mbB
Brienner Str. 13, D-80333 Munich
- info@darmsprechstunde.de
- Monday - Friday: 08.00 - 13.00 and 14.00 - 18.00
- and by arrangement
- Saturday, Sunday, Holiday : closed
- Please also note our instructions in the title of this website and on our telephone announcement.
© 2023 Proctology Practice Munich
