Steißbeinfistel - Sinus pilonidalis?
Endlich wieder frei von Schmerzen, Blutungen und unangenehmen Gerüchen werden
Habe ich überhaupt eine Steißbeinfistel?
- Was ist eine Steißbeinfistel?
- Welches sind die typischen Symptome eines Sinus pilonidalis?
- Wie kann eine Steißbeinfistel aussehen?
Ignorieren? Operieren? Und wenn ja, wie?
- Möglichkeiten der Behandlung ohne OP
- Operationsmethoden bei Steißbeinfistel
- Vorteile der Laser – Behandlung und Laser – Operation
Ich wurde schon operiert. Die Fistel ist wieder da. Was tun?
- Warum kommt es zu einem Rückfall (Rezidiv)?
- In welchen Fällen kann man beim Rezidiv minimal-invasiv behandeln?
- Wann empfiehlt sich eine Karydakis Operation?
Sinus pilonidalis - Was ist das?
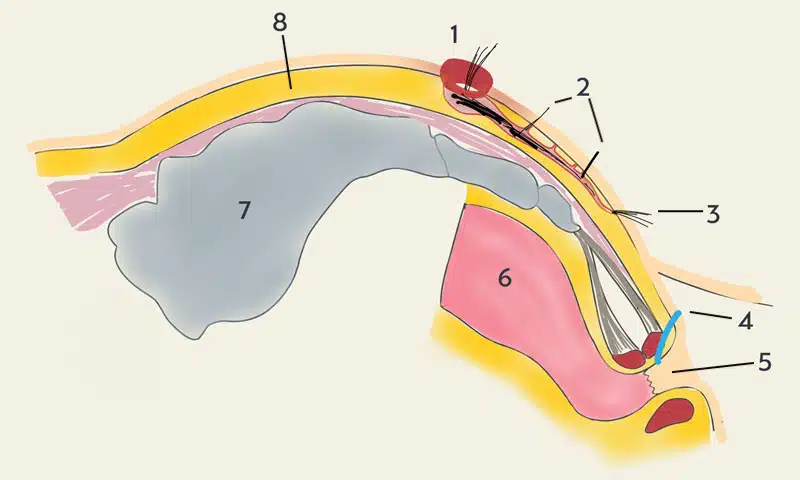
Mayo beschrieb das Krankheitsbild erstmalig im Jahr 1833. Der Begriff Fistel (lat. fistula Röhre, Pfeife) bezeichnet einen röhrenförmigen Gang als Folge einer chronischen Entzündung. Der Begriff Sinus pilonidalis ( Pilonidalsinus, Pilonidalzyste, Steißbeinzyste, Sakraldermoid, Dermoidzyste) stammt von Hodge 1880 (lat. pilus = Haar und nidus = Nest).
Diese Fisteln findet man nur in der Gesäßfalte. Sie kann chronisch (= Steißbeinfistel) oder akut (= Steißbeinabszeß) sein. Eingewachsene oder eingespießte Haare führen als Fremdkörper zu einem Reizzustand. Es bildet sich ein Schutzwall aus Narbengewebe, die Fistelkapsel (Fremdkörpergranulom).
Eine stabile Schicht aus kollagenem Bindegewebe, die Faszie, schützt den Gesäßmuskel und das Steißbein.
Der Enddarm und der Schließmuskel sind nie betroffen.
Der Pilonidalsinus ist eine einfache Erkrankung.
1992 George E. Karydakis, griechischer Chirurg und Begründer des asymmetrischen Wundverschlusses bei der Operation der Steißbeinfistel, Anz Journal of Surgery, 62(5), 385-389.
Zu welchem Arzt geht man am besten?
Warum braucht man bei einer einfachen Erkrankung einen Spezialisten?
Die Steißbeinfistel ist eine Hautkrankheit. Folgerichtig wäre der Dermatologe zuständig. Erster Ansprechpartner ist aber meist der Hausarzt. Er überweist den Patienten an den Chirurgen.
In Deutschland werden jährlich etwa 50.000 Patienten am Sinus pilonidalis operiert. Anders ausgedrückt: Jeder Chirurg behandelt durchschnittlich nur 1,4 Patienten mit einer Steißbeinfistel pro Jahr. Bei dieser Fallzahl ist es schwierig, Erfahrung zu sammeln.
Suchen Sie sich einen Arzt, der mit seiner Methode wirklich viel Erfahrung hat und sich schwerpunktmäßig mit der Behandlung von Steißbeinfisteln beschäftigt. Wählen Sie nicht das nächstgelegene Krankenhaus, nicht den schnellsten Termin, nicht den Arzt mit dem allgemein besten Ruf, sondern den besten Arzt für Ihr Problem.
Steißbeinfistel - OP: Wo ist das Problem?
Der vermeintlich kleine Eingriff kann unerwartet große Folgen haben.
- Lange Heilungsdauer mit Krankschreibung
- Aufwändige und schmerzhafte Wundbehandlungen,
- häufige Wundheilungsstörungen
- hohe Rückfallrate bis 57 % (Deutsches Ärzteblatt 2019)
- Aufreißen der Narbe
- Wiederholte Krankenhausaufenthalte
- Einkommensverlust und Karriereknick
- Einschränkungen der sportlichen Fitness, Gewichtszunahme
- Einschränkungen des Körpergefühls und der Sexualität

Gute Entscheidungen gründen auf Erfahrung.
John U. Bascom M.D., Pionier der modernen Operation der Steißbeinfistel, Eugene/Oregon U.S.A., 1925 - 2013
Wir sind die Experten
6123
Operationen bei Steissbeinfistel (Stand 29.03.2023)
8763
Behandlungsfälle bei Steissbeinfistel (Stand 14.04.2022)
Laser
Erfahrung in Laser-Therapie und Laser-Chirurgie seit 2012
Kasse und Privat
Volle Zulassung für ambulante Operationen und integrierte Versorgung
Pit Picking Operation - Die schonende Alternative
Eine Heilung der Steißbeinfistel ist nach heutigem Stand der Wissenschaft nur durch eine Operation möglich. Die Faktoren, die über Erfolg oder Misserfolg einer Operation entscheiden, wurden bereits 1965 von dem englischen Chirurgen Peter Lord beschrieben.
- Die Ursache der Steißbeinfistel sind in das Unterhautgewebe eingewachsene Haare.
- Alle eingewachsenen Haare müssen vollständig entfernt werden.
- Alle Eintrittspforten (Porus, Pits) für Haare müssen identifiziert und beseitigt werden.
Diese Ziele können in der Regel durch eine relativ einfache und kleine Operation erreicht werden.
Alle Fisteln werden heilen, wenn sie nicht offengehalten werden. Ein Pilonidalsinus ist eine Fremdkörper - Fistel, wobei Haare der Fremdkörper sind. Wenn die Haare entfernt werden, wird die Fistel heilen
Peter H. Lord und Douglas M. Millar, Begründer der Pit Picking Operation für die Steißbeinfistel, BRIT. J. SURG., 1965, Vol. 52
Operationstechniken
Ausschneidung mit offener Wundbehandlung ("Metzger-Methode")
Die Geschichte der Operation der Steißbeinfistel beginnt mit einem Irrtum.
Als Anfang des vergangenen Jahrhunderts die Diagnose des Sinus pilonidalis zunehmend häufig gestellt wurde, unter anderem bei Soldaten im Ersten Weltkrieg („Jeep’s Disease”), dachte man an die angeborene Erkrankung einer embryonalen Fehlbildung.
Anders ausgedrückt, könnte es nach einer vollständigen Entfernung nicht zu einem Rückfall (Rezidiv) kommen. Nachdem aber dennoch Rezidive beobachtet wurden, wurde das Ausmaß der Operationen immer weiter ausgedehnt.
Diese radikale Entfernung (lateinisch ‘radix’, Wurzel) setzte sich weltweit durch. Obwohl diese Theorie seit Patey als widerlegt gilt, halten die meisten Chirurgen bis heute an diesem überholten Therapiekonzept fest.
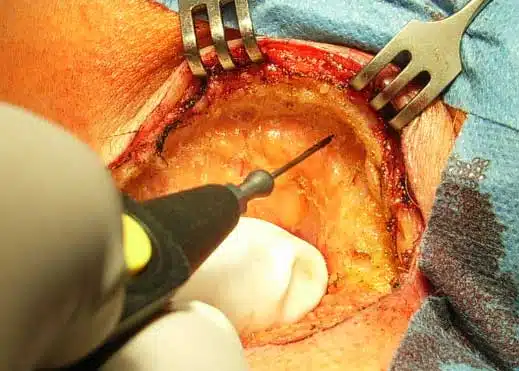
Ausschneidung mit Verschluß der Wunde durch Eigengewebe (Lappenplastik)
Warum näht man die Wunde nicht zu?
Bei einer einfachen Naht in der Mittellinie sind Wundinfektionen häufig, die Naht platzt auf oder muß wieder geöffnet werden.
Zudem führt die Naht zu einem leichten Einstülpen (Inversion) der Wundränder, was das erneute Einwachsen von Haaren und damit den Rückfall (Rezidiv) begünstigt.
Die ständigen Bewegungen beim Gehen und Sitzen verursachen Scherkräfte im Bereich der Gesäßfalte, die eine stabile Heilung einer genähten Wunde verhindern.
Deshalb wurden Verfahren entwickelt, die durch Verlagerung von Eigengewebe (Lappenplastik) die Spannung in den Nähten vermindern und eine zur Seite verlagerte (medizinisch: lateralisierte) Naht ermöglichen sollen:
- Karydakis – Operation
- Limberg – Operation und die verwandte Dufourmentel – Technik
Die Alternative
Pit Picking Operation, Laser – OP (SiLaC®), Sinusektomie, Endoskopie (EPSiT)
Weniger ist mehr:
Basierend auf der in England entwickelten und in den USA populär gewordenen Pit-Picking-Technik stehen verschiedene Varianten dieser schonenden Behandlung zur Verfügung.
Unter Pit-Picking versteht man die selektive Entfernung der betroffenen Haarwurzeln als Hautzylinder von 2-5 mm Durchmesser und die Reinigung des Fistelganges von abgelagerten Haarfragmenten.
Je perfekter dies gelingt, desto geringer ist das Risiko einer erneuten Fistelbildung.
Die Entscheidung, welche Technologie am besten geeignet ist, muss individuell getroffen werden:
- Laserbehandlung der Fistel von innen mit einer Glasfasersonde (SiLaC®)
- Präzise Ausschälung entlang der Fistelkapsel (Sinusektomie oder Fistulektomie).
- Videoendoskopische Operation (Endoscopic Pilonidal Sinus Therapy EPSiT)


Nachbehandlung nach der Operation
Bei uns werden Sie nach der Operation nicht alleine gelassen.
Die beste Operation garantiert noch keine problemlose Heilung. In Fragen der Nachbehandlung beraten wir Sie bereits beim Operationstermin.
Gerade wenn Sie weiter entfernt wohnen, kann so aus Ihrem Angehörigen ihr privater Wundspezialist werden. Wir unterstützen Sie dabei durch alle gängigen, digitalen Kommunikationskanäle.
Aus unserer Informationsbroschüre erfahren Sie, was sie im Verlauf zu erwarten haben.
Beim Nachsorgetermin in der Praxis kümmert sich Ihr Operateur bei Bedarf persönlich um den optimalen Heilverlauf.
In unserer speziellen Wund- und Laser – Sprechstunde wird ihre Wunde durch eine geschulte und erfahrene Therapeutin professionell gepflegt.
Die Erfolgsgeschichte unserer Praxis
Post von Dr. John Bascom aus Eugene, Oregon
Das muss ungefähr 2003 gewesen sein. Nach bestandener Facharztprüfung durfte ich selbständig operieren. Die ersten Eingriffe, die auf einen jungen Chirurgen warten, sind die vermeintlich einfachen – wie die Entfernung einer Steißbeinfistel.
In der Facharztausbildung lernte ich die heute von vielen Patienten als „Metzger-Methode“ bezeichnete vollständige Entfernung der Fistelregion bis auf den Knochen.
Mein Freund und Kollege Dr. K. mußte nach einer solchen Operation in einer großen Münchner Klinik eine 9 Monate dauernde schmerzhafte Wundbehandlung am eigenen Leibe erfahren.

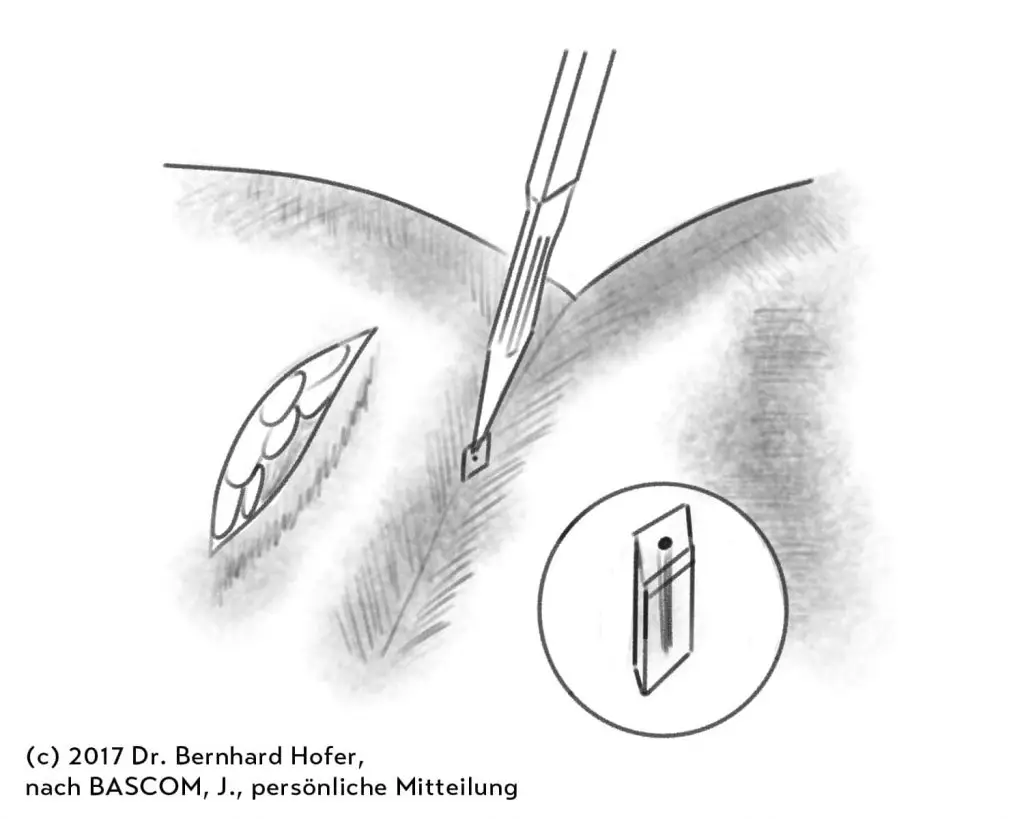
Eine revolutionär neue Methode aus England und den USA
„Das muss doch irgendwie anders gehen“, waren seine Worte, die mir im Gedächtnis blieben.
Während meiner Recherche im damals aufkeimenden Internet stieß ich auf die Methode von Dr. John Bascom aus den USA. Obwohl der eigentliche Erfinder der britische Chirurg Dr. Peter Lord war, machte Bascom die „Pit Picking“ – Operation weltweit bekannt.
Ein herzliches Dankeschön geht an John Bascom für seine unschätzbare Hilfe und Unterstützung! Als Pionier der Pit Picking Methode schickte er mir ein Päckchen mit Anleitungen, einer Video-CD und selbstgezeichneten Grafiken. In schwierigen Fällen konnte man jederzeit einen guten Rat per E-Mail von ihm erhalten.
Evolution der Pit Picking Technik Operation
Trotz einer Erfolgsrate von anfangs nur etwa 50 % waren die Patienten glücklich, der Standardoperation entkommen zu sein. Folglich kamen immer mehr Anfragen. Die Optimierung der Operationstechnik durch innovative Technologien, feine Spezial-Instrumente, nützlichen Medikamenten und Biomaterialien verbunden mit der Erfahrung aus mittlerweile über 6000 Operationen konnte die Ergebnisse kontinuierlich verbessern.
Heute erreichen wir Heilungsraten von > 90 %. Aktuell suchen etwa 1000 Patienten pro Jahr mit einer Steißbeinfistel unsere Praxis auf.
Daraus haben wir gelernt, dass minimal-invasive Techniken nicht nur für eine Erstoperation geeignet sind. Auch dem Rückfall (Rezidiv) kann man damit die Schrecken nehmen.